As the central feature of one’s face, the nose is arguably the most important structure in determining identity, and influencing the balance and harmony of the face. So, it is easy to see why nasal deformities, however minor, can affect facial beauty. In addition, nasal shape can affect function as well as form, given the nose’s significant role in breathing. We feel that nose surgery should therefore be performed only by facial plastic surgeons, who are specialists in nasal anatomy, function, and aesthetics. This section will introduce you to the history and classifications of rhinoplasty, and summarize the complexity of nasal structure. You will also see how rhinoplasty, when performed by skilled hands, can create the harmonious, natural, and functional rhinoplasty result you desire.

Types of Rhinoplasty
As you begin the evaluation process for rhinoplasty surgery, you will undoubtedly hear many new terms and concepts. Having an understanding of basic rhinoplasty classifications will therefore help you to better comprehend all that you will learn, and will make the process more enjoyable.
In general, nasal surgery is described as either “closed” or “open”. These terms refer to the placement of incisions – closed rhinoplasty incisions are completely hidden inside the nostrils, whereas open rhinoplasty also includes an incision made in the skin between the nostrils. You may also hear thete terms “primary” rhinoplasty, referring to the first nasal procedure, and revision rhinoplasty, implying that you have had at least one rhinoplasty in the past. Revision procedures are often more complex given existing scar tissue, and are more likely to require an open technique. You should also consider if you desire a purely “aesthetic” correction, or if your complaints are mainly “functional”. For many of our patients, improving the aesthetic and functional components of the nose is required.
Suitable Patients for Rhinoplasty
Many patients seeking rhinoplasty have purely cosmetic complaints, such as a crooked or deviated nose, a large tip, a hump or depression along the bridge of the nose, wide nostrils, or a nose that is too narrow or wide. Patients may also complain that they are unable to breath well through one or both sides of the nose, or have had trauma to their noses. If you have any of these complaints, you are most likely a suitable patient for rhinoplasty.
Issues that do not relate to the nose also affect suitability. Ideal patients should be in good health, and should be able to avoid blood thinning medications around the time of the surgery. To ensure completed facial growth, patients should be past adolescence; for women, this is usually after the age of 16, and for men it is usually after age 18. Patients with severe seasonal or environmental allergies are sometimes not candidates for rhinoplasty, but our doctors can discuss this with you during your consultation.
History of Rhinoplasty
The field of rhinoplasty began almost exclusively with reconstructive procedures. The earliest description of nasal surgery was made almost 5,000 years ago in an Egyptian surgical treatise, and involved the repair of nasal fractures. In 600 B.C., an Indian holy book reported the repair of severed noses using cheek skin flaps, which was common given the use of nasal mutilation as punishment. Interestingly, these early Indian facial surgeons were actually tile makers. By the 19th century, many reports had been published on the use of prosthetic noses (made of silver, aluminum, bone, and other materials), forehead and other facial skin flaps, arm skin flaps, and chest skin flaps to repair the traumatized nose.
Rhinoplasty for purely cosmetic purposes was much later in its development. In 1845, a procedure for straightening a crooked nose was proposed by a European surgeon, Johann Dieffenbach, and in 1887 an American doctor named John Roe described the reduction of a “pug nose”. However, the true father of modern cosmetic rhinoplasty is a German physician named Jacques Joseph. In 1907, his Treatise on Rhinoplasty extensively detailed nasal deformities and their respective surgical treatments. Some of these procedures, and several of Dr. Joseph’s instruments, are still being used by rhinoplasty surgeons today.
I first came to Dr. Kabaker 25 years ago and had my eyelids and rhinoplasty surgeries. I am very happy with the results. I feel he is an excellent surgeon who is very professional, with wonderful skills and caring. I just recently returned after noticing that I was looking tired, and had a face and neck lift procedure, and a lip implant. I would not hesitate to recommend Dr. Kabaker for any of the procedures that I can attest to. He and his staff are friendly and truly caring. P.S. He has also done some fantastic hiding of old scars from a car accident!
Nasal Anatomy
The nose is made of many types of tissue, which makes rhinoplasty especially difficult for the untrained surgeon. The nasal framework consists primarily of cartilage, which forms the lower two-thirds of the nose and the anterior septum. Complexity is created by the many individual pieces of cartilage, their unique shapes, and the strong connective tissue that holds them together. Bone is also important, forming the upper one-third of the nose and posterior septum. The nose also has the pink, moist tissue on the inside – the “mucosa” – and several small muscles that affect its shape. Most, if not all, of these tissues need to be altered during a rhinoplasty surgery, so the skin will lay down over them in consistent manner, and the nasal appearance and function will improve.
The Consultation
When you arrive at our San Francisco office, you will be asked to complete a detailed questionnaire about your medical and surgical history. Dr. Kabaker will then take standardized photographs, and examine the outside and inside of your nose. Most importantly, you will be given ample time to describe your complaints, and to learn about your proposed procedure and how it might help you. Our doctors will also use a state of the art computer photo alteration program to predict your surgical outcome.
As mentioned elsewhere in this website, we stress patient education. So, during the consultation, you will learn a great deal about the anatomic considerations that cause your complaints, how they will be changed, what you will experience during the recovery, and your risks and alternatives to treatment. You will be given much information in writing, and we are always available for a second consultation, if you wish to review anything.
The Pre-operative Process
For the two weeks prior to your procedure, you should refrain from using common medications that decrease your blood’s ability to clot, including aspirin, ibuprofen, Advil, Motrin, Bufferin, Naprosyn, and large doses of vitamin E. Our doctors will give you specific instructions based on your current medications. If you have any headaches or other pain, taking acetaminophen (Tylenol) is fine. You should also avoid smoking for two weeks before your surgery. The night before your surgery, you should eat a normal dinner but avoid all oral intake after midnight. This includes drinking anything, even water.
When you schedule your rhinoplasty, you will be given a detailed set of instructions that includes much more information. A copy of these Rhinoplasty Instructions is available for you to review now.
Your Procedure
It is often said that a surgeon has three chances to evaluate a nasal patient; the first two are the consultation and the immediate pre-operative checkup. However, it is during the procedure that the most important treatment decisions are made. By directly examining your nasal anatomy, Dr. Kabaker will determine the changes necessary to creating a better nasal shape – one that fits your overall facial structure, your chin position, your cheeks and eyes, and your forehead shape. Anatomic blockages to your breathing can also be corrected.
You will need to arrive about two hours prior to the start of your procedure. The procedure itself will take approximately two to four hours, depending on the technique used. You will stay in our recovery room one to two hours, and then you will be able to return home. You will need a companion to accompany you when leaving our surgery center.
Anesthesia
Most rhinoplasty patients receive a deep sedation, which means they are completely asleep during the procedure but are breathing on their own, so there is no need for a breathing tube. This type of anesthesia is always provided by a highly qualified doctor or nurse anesthetist, who will be dedicated to the anesthetic treatment for the entire case. Other patients can have a more shallow sedation or even just local anesthetic, but they are usually having very short procedures. No matter what, every patient will be completely comfortable and the procedure itself will be pain-free.
Rhinoplasty Recovery
Most patients fear that the post-operative experience after rhinoplasty is painful. This is not true! Almost all patients are pleasantly surprised with their level of comfort. You will be provided pain medication and other suggestions to minimize your soreness. Most patients report a mild burning sensation inside the nostrils, from healing incisions. If the bones of your nose need to be reset, then you may experience mild mid-facial soreness by the second or third day.
After rhinoplasty, patients have small gauze wicks in each nostril for one day, so you will need to return to the office the day after surgery to have them removed. The wicks cause nasal obstruction for the first day, but upon removal the nasal airways open. You will also have a small plastic cast on your nose after surgery, and you will return to the office one week after surgery to remove this cast. If your procedure was done with the “open” technique, you will have your skin sutures removed at this visit. If you had the “closed” technique, there are no sutures to remove.
You will have mild drainage from the nose for two to three days, and may have bruising under your eyes that should resolve after 7 to 10 days. You will have swelling of the cheeks that will also last about one week.
One of the biggest challenges for patients after rhinoplasty is waiting for the nasal swelling to resolve. While swelling of the top of your nose will last about two weeks, the swelling of the tip of your nose will require months to resolve. This can be quite frustrating for patients who are anxious to see the “final result”, but swelling is absolutely unavoidable after rhinoplasty. You will have to be a “patient patient”, and not get pre-occupied with the appearance of the tip too early.
FAQs about Rhinoplasty
If you have further questions about rhinoplasty, check the list below to find answers. While some information presented here is also contained in the above text, these short responses should complete your introduction to rhinoplasty. We also encourage you to consult with Dr. Kabaker for individualized answers to all of your questions.
Am I a good candidate for rhinoplasty?
The best rhinoplasty patients are in good health, over the age of 16, non-smokers, and are able to avoid blood thinning medications for two weeks before surgery. They have complaints with nasal appearance and/or breathing, and have realistic expectations of the result. They are able to understand the basic aspects of rhinoplasty so they can easily participate in their own care.
How do I choose a rhinoplasty surgeon?
There are many good rhinoplasty surgeons available, so choosing the best one for you is a challenge. Your surgeon should listen well to your requests and not tell you what you need. He or she should educate you enough to help you understand what you are going through, but not overload you with information. He or she should only promise realistic results. He or she should work toward creating a natural and improved look for your nose, and not necessarily a “perfect” nose as suggested by magazine advertisements or celebrities.
How many doctors should I consult with?
As many as you need to feel completely comfortable with the doctor you choose. Some patients are able to settle on their surgeon after only one consultation, while others require several to best compare their rapport with each doctor.
Is a surgeon’s experience important?
It certainly is. We think your surgeon should be someone who only operates on the face, and has done enough rhinoplasties to master all available techniques. We think the age of a surgeon is not important; only his or her ability to translate your requests into results matters.
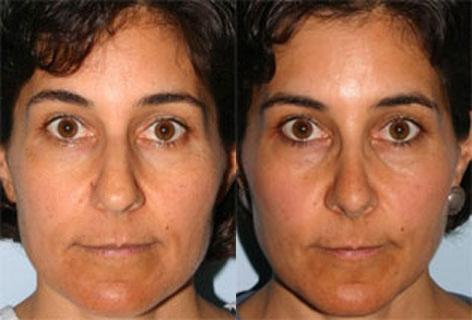
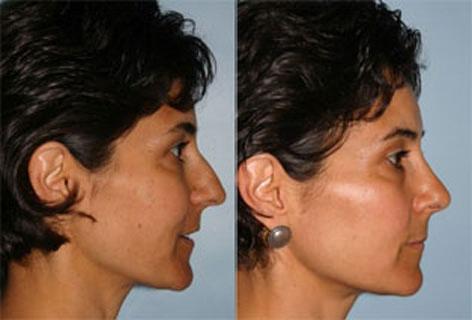
Are “before and after” pictures helpful?
They are, and our doctors will show you many. But, remember that you are the only person with your exact nose. Every patient is different, so try not to base your decision on before and after photos. You should focus more on what the surgeon will do for you as an individual.
Do you use computers to change my pre-operative photos?
Yes, we do, and we use the latest software available to provide realistic projections. Keep in mind that these “morphed” images are not guarantees of an actual result, but will help you as you plan your procedure.
Is rhinoplasty expensive?
Having a rhinoplasty is like investing in your self-image and confidence, so while the financial cost is not low, the rewards can be great. The actual cost of your procedure will depend on exactly what is done, and a written quote will be given to you. We promise, though, that the overall value of your procedure will be competitive and fair. Costs for dedicated facial plastic surgeon like Dr. Kabaker reflect their dedication to this specific field, and we feel that you should not emphasize cost savings when dealing with your face.
Do I need to see my own doctor before a rhinoplasty?
All patients require basic lab tests, and typically patients over the age of 45 require a written clearance from their personal physicians. All specific requirements are described in the attached Rhinoplasty Instructions.
What do I need to do the day before surgery?
The day before a rhinoplasty, you should eat normally but avoid excessively heavy meals, or foods that can lead to acid reflux. Prepare your affairs so that you completely relax and rest after surgery. Most importantly, do not eat or drink anything after midnight before your procedure. See the attached Rhinoplasty Instructions for all suggestions.
Where does the surgery take place?
Procedures are done at the Aesthetic Facial Plastic Surgery Our Clinic, our fully accredited surgery center.
What kind of anesthetic will be used?
For almost all cases, a deep sedation will be used, which means you will be completely asleep and pain-free during the entire case. No breathing tube will be needed in these cases. Some other patients, having shorter procedures, can have lighter sedation. However, everyone will be completely comfortable during the procedure.
Can I wake up in the middle of surgery?
No. If you are having a deep sedation, an anesthetic professional (anesthesiologist or nurse anesthetist) will be dedicated to providing anesthesia during the entire case.
How long does the procedure take?
Primary rhinoplasties are usually done with a closed approach, and take 1 ½ to 2 hours. Revision procedures may take up to 4 hours and often require an open approach.
How much pain will I have after surgery?
Not as much as you probably think! We have found that most patients are very worried about pain, and pleasantly surprised to find that discomfort is mild. The biggest complaint most patients express is nasal obstruction from gauze wicks in each nostril, but these are removed the day after surgery and the obstruction is thus resolved. Pain is usually well controlled with medications, which we will prescribe.
What kind of nasal packing is used after the procedure?
None. There will be a small gauze wick in each nostril, and these are removed the morning after surgery. This removal is not painful, so patients should not over treat themselves with pain medications before this office visit.
What are the risks of surgery?
Adverse events are rare and mild. One possible risk is bleeding. All patients have nasal drainage for a few days after surgery, and early on this may be “blood tinged” – pink in color, but not a true nose bleed. Approximately 2% of patients will actually have blood slowly oozing from a nostril, and this is easily controlled at home. We will show you how during your evaluations. A severe nosebleed, requiring our intervention, is extremely unlikely. Another risk of surgery is excessive scar formation. This is also very rare, and usually seen as a hard bump in the nasal bone, or a softer bump at the nasal tip. For the approximately 2% of patients who experience this, the problem is easily correctible. Such scar tissue does not reflect poor surgical technique – it is true that some patients are just prone to a robust healing response.
Will I be swollen?
Swelling is impossible to avoid. Your cheeks will be swollen for approximately one to two weeks after surgery, but this is often only noticeable to the patient. Your nasal skin, though, will be swollen for longer, and this is extremely important for patients to remember. It may take months for the swelling at the tip of your nose to resolve, and the “final result” will not be seen until the swelling is gone. This waiting period can be frustrating for some patients. We will give you many suggestions about minimizing swelling, and helping it to resolve as quickly as possible.
When will the results of my rhinoplasty be visible?
Though it will be swollen, your nose will look more aesthetically pleasing and natural immediately after surgery. You will first see this as soon as your plastic splint is removed (after one week). And, once all bruising is resolved, there will be no adverse signs of surgery – only a better nasal structure that continues to improve as healing progresses.
Will I have scars?
If your procedure is done with the “closed” technique, then all incisions are inside the nose and no scars are created in your skin. If you have the “open” technique, then there will be a very small, unnoticeable scar in the skin between your nostrils.
How much time off should I take from school/work?
At least one week is recommended. The plastic splint on your nose will be removed after seven days, leaving you free of this obvious stigmata of surgery. You may still be mildly bruised under your eyes, so if this will interfere with your work or school, then it may be safer to take two weeks off.
What precautions should I take after surgery?
You should avoid contact to your nose for about two months after surgery. Also, any strenuous activities or exercise during the two or three weeks after surgery will increase your swelling, so should be avoided. We understand it is often difficult to abstain from exercising during this time, but you should consider this an important investment in your outcome. Wearing heavy glasses should be avoided for several weeks. Lastly, avoid excessive heat or sun exposure for the month after surgery.
Do patients ever need another rhinoplasty?
While very uncommon, some patients will want slight changes to be made after a primary rhinoplasty. Often, these secondary complaints are the result of the healing process, and not mistakes that were made during the primary surgery. In any case, we insist on satisfying our patients, and want you to be completely happy with your rhinoplasty outcome. We will take necessary steps to correct any post-operative complaints if they arise. Occasionally, patients need a surgical correction, and we do not charge surgery fees if such correction is done up to eighteen months after the primary procedure. Patients are responsible, though, for operating room and anesthetic fees for the revision procedure.